On May 26, 2021, the New York Times made the last update to its COVID-19 tracker for U.S. colleges and universities — the first full school year since the pandemic began had come to an end. The University of Wisconsin-Madison may not have medaled for most cases of coronavirus in the country, but it did come in fourth with 7,708.
Pre-delta, the university’s rates of COVID-19 exploded when students returned to campus. It joined the ranks of COVID frontrunners such as Ohio State, the University of Florida and Indiana University-Bloomington. The NYT also found itself covering UW-Madison again amidst the shutdowns of two of its largest dormitories. Without a vaccine mandate, and fewer precautions and restrictions taken than last spring, the university almost seems like it's marching head-on towards a repeat of last fall.
There is still hope: UW has reached a 90% vaccination rate among its campus population and will be requiring masks indoors. But will it be enough?
Ajay Sethi, an expert in epidemiology and population health and associate professor at UW-Madison, believes that the university is well prepared for an in-person fall semester, but that it may see some hiccups along the way.
“We don’t know how [delta] spreads exactly; we do know it spreads a lot in comparison to other variants,” Sethi said. “Infected individuals put out more of the virus and that will affect how it spreads.”
Sethi pointed to last fall’s outbreak, noting that if the university does experience a similar spread of the virus as classes resume, that it may be able to get a handle on its case numbers by the winter. However, with the delta variant in play, these cases may be more resistant.
He also noted that achieving a high rate of vaccination among students will no longer be enough to ensure that “herd immunity” is reached on campus. Herd immunity entails protection from infectious disease that can occur when a big enough percentage of a population becomes immune to infection through vaccination or previous infections. As long as current vaccines do not stop the virus entirely, achieving this level of immunity when the highly infectious delta variant is spreading is not likely to happen.
Because of this, Sethi believes that the virus is not going to disappear any time soon.
“At this point, there is no such thing as herd immunity,” he clarified. “I actually have discouraged the use of the phrase because we just aren’t going to reach that.”
Troubles may arise if cases increase too quickly; the university has limited isolation facilities and far fewer options for COVID-19 testing this fall. Testing appointments need to be made in advance and nose swabs can take as long as 30 hours to provide results — a sharp contrast to last year’s spit tests and 4 to 6 hour results.
One way to avoid another catastrophe is frequent testing by the vaccinated campus community. While the university only requires weekly testing for the unvaccinated, this is not sufficient thanks to the delta variant. Testing can catch what students may have disregarded as cold symptoms or identify those that are asymptomatic. Sethi also emphasized the importance of the use of space in classrooms and even outdoors; social distancing is the best tool to ensure that spread is limited. He added that spacing may be even more important to stopping delta than testing.
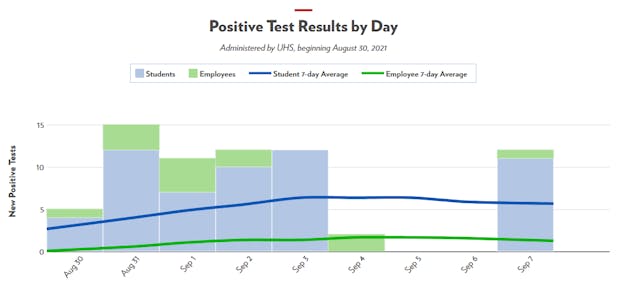
Currently, the UW-Madison COVID-19 Dashboard lists the university’s 7-day average at 6.4 students testing positive daily. On Sept. 7, the first-day reporting test results after a long Labor Day weekend and a home game for the Badgers, 11 students tested positive. In comparison, 290 students tested positive on Sept. 9 last year after a similar quiet period with few positive tests. Vaccines and masks may not halt the virus, but it will certainly be able to slow it down.
Looking to the future, UW-Madison is well-equipped to respond to delta and mitigate its relatively small caseload. Let’s keep our fingers crossed that it stays that way.
Addison Lathers is the Editor in Chief of The Daily Cardinal. She has covered city and campus news and held two editor positions. Follow her on Twitter at @addisonlathers.






